Quick Facts
- Category: Health & Medicine
- Published: 2026-05-07 00:30:09
- 8 Things You Need to Know About Dark and Darker's Legal Victory Over Nexon
- Modernize Your Go Code with go fix: A Q&A Guide
- SUSE Unveils AI-Native Infrastructure Layer for Enterprise Clouds at KubeCon Europe 2026
- GitHub Copilot Transitions to Usage-Based Billing: Key Changes and Timeline
- 10 Incredible Facts About the Many Phases of Ice
For decades, arthroscopic partial meniscectomy—a procedure to trim a torn meniscus—has been one of the most performed orthopedic surgeries worldwide. Yet a groundbreaking 10-year clinical trial now turns this practice on its head, suggesting the operation provides no real advantage over a placebo and may even worsen patients' long-term outcomes.
Understanding the Meniscus and Its Role
The meniscus is a C-shaped piece of cartilage in the knee that acts as a shock absorber and stabilizer. When torn—often from twisting injuries or age-related degeneration—patients typically experience pain, swelling, and limited motion. For years, the standard surgical response has been to remove the damaged portion, known as partial meniscectomy, with the goal of relieving symptoms and preventing further joint damage.
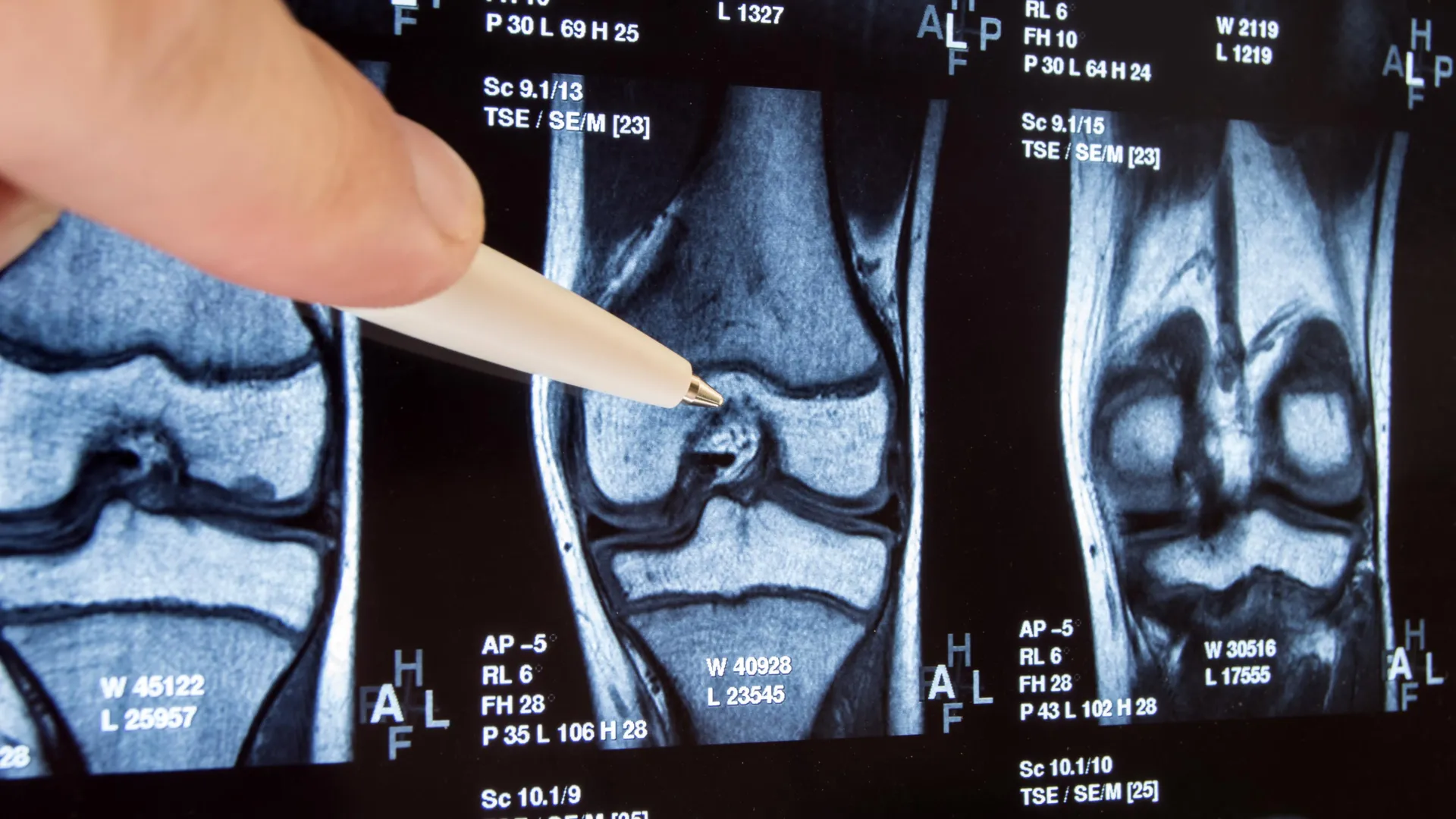
The Surgery in Question: Arthroscopic Partial Meniscectomy
Performed through small incisions with a camera and instruments, arthroscopic meniscectomy is minimally invasive and has a relatively quick recovery. Surgeons worldwide have performed millions of these procedures, believing that trimming the frayed edges would reduce friction and pain. But recent evidence has raised questions about its efficacy, especially in patients with degenerative (age-related) meniscal tears—a common finding in older adults with no acute injury.
The 10-Year Clinical Trial That Changed the Picture
Researchers conducted a randomized, placebo-controlled trial spanning a decade, comparing arthroscopic partial meniscectomy with a sham surgery (placebo) where patients underwent the same incisions and recovery but no actual meniscus removal. The results, published in a leading medical journal, were striking:
No Better Than Placebo
At both short-term (two years) and long-term (five to ten years) follow-ups, patients who received the real surgery reported similar levels of pain and knee function as those who had the placebo procedure. In other words, the act of trimming the meniscus added no measurable benefit beyond the placebo effect of surgery itself.
Worse Long-Term Outcomes
Surprisingly, patients who underwent the actual operation fared worse over time. They experienced:
- More persistent symptoms, including pain and swelling
- Poorer knee function during daily activities and exercise
- Faster progression of osteoarthritis, as seen on X-rays and MRI scans
- Higher likelihood of needing additional surgery, such as a knee replacement, within the follow-up period
These findings suggest that removing even a small part of the meniscus may destabilize the joint and accelerate cartilage wear, leading to earlier and more severe arthritis.
Implications for Patients and Surgeons
The trial challenges long-held surgical dogma. For patients with a degenerative meniscal tear and no clear injury, the evidence now strongly supports non-surgical approaches first. Options include physical therapy, activity modification, anti-inflammatory medications, and corticosteroid injections. Only in cases of a locked knee or significant mechanical symptoms—like catching or locking—should surgery be considered, and even then, the expected benefits may be modest.
Surgeons are updating guidelines, and many now emphasize shared decision-making. Patients should be informed that the 10-year trial shows this common operation may not only be ineffective but could also hasten joint deterioration.
Alternatives to Arthroscopic Meniscectomy
Several effective, non-surgical treatments can manage meniscal tear symptoms:
- Physical therapy: Strengthening the muscles around the knee (quadriceps, hamstrings, calves) improves stability and reduces pain.
- Activity modification: Avoiding high-impact activities like running or jumping can prevent irritation.
- Medications: Nonsteroidal anti-inflammatory drugs (NSAIDs) and acetaminophen can control pain and inflammation.
- Injections: Corticosteroid or hyaluronic acid injections may provide temporary relief.
- Weight management: Reducing body weight decreases stress on the knee joint.
For patients who do not improve, repair of the meniscus (meniscal repair) remains an option for certain types of tears, though it requires a longer recovery and may not be suitable for all.
Conclusion
This pivotal study underscores that more surgery is not always better. The findings call for a paradigm shift: arthroscopic partial meniscectomy for degenerative tears should be used sparingly, if at all. Patients and doctors alike should weigh the evidence of potential harm against the unproven benefits. For most, conservative care offers a safer path forward.